Regulatory news
We have just published our annual report. Find out more about our work reviewing the regulators in the full report or in our highlights.
Lessons Learned Review of the Nursing and Midwifery Council published
In May we published our review of the NMC’s handling of concerns about midwives at the Furness General Hospital Morecambe Bay. There had been problems at the midwifery unit in that hospital since at least 2004, including the tragic deaths of babies and mothers. The NMC had first become aware of the concerns in 2010 but did not complete the fitness to practise hearings until June 2017. The Secretary of State commissioned us to undertake the review to see whether lessons could be learned.
We began the review in July 2017 and considered over 60 cases and many thousands of documents. Our review found that there had been considerable serious failings in the NMC's investigation and prosecution of the cases, particularly in the early stages. We found that evidence provided by the families was not looked at clearly, that there was inadequate clinical advice and poor analysis of the complaints. We also found that the NMC did not engage well with the families and that it was not transparent with them.
We also noted that the fitness to practise process was not well placed to deal with situations such as this, particularly where there were real concerns about the attitude of the Trust as well.
We found that the NMC had improved significantly since many of the problems occurred. It had processes which were likely to address many of the issues we raised. However, we were still concerned about the way in which it continued to treat families and patients and by a lack of transparency – particularly over a Subject Access Request by one of the families. We consider that the NMC needs to address these as a priority. We will monitor the NMC’s progress with this through our performance reviews.
You can read the full review on our website as well as our latest performance review of the NMC.
Scrutinising final fitness to practise decisions
A case study: how the process works within the Authority
If you read the key statistics from our latest annual report, you will see that we receive around 4,200 final fitness to practise decisions each year.
This is just a statistic but behind this statistic are stories involving real people – health professionals and their patients. Our process involves members of our Scrutiny and Quality team reading through some heartbreaking and harrowing details, but fitness to practise is a legal process and it is always important to remain detached and make an objective assessment of the case, with our prime focus being the public interest.
Our role (powers given to us under Section 29 of the Health and Social Care Act) is to check that all the regulators’ fitness to practise decisions are sufficient to protect the public and that regulators’ panels have adhered to the legal technicalities of the process. In about 85 per cent of these cases, no further action is required. We hold detailed case reviews for an average of 250 decisions every year.
There is much misunderstanding around the fitness to practise process. It is not a process for assigning blame or seeking justice but, focusing on whether the registrant who is the subject of this process, is fit to practise at the time the decision is made (which can sometimes be well after the initial incident has occurred).
One of these cases involved Dr Valerie Murphy – a registrant of the General Medical Council. We considered this case in April 2018. Dr Murphy was the consultant psychiatrist at a short-term assessment and treatment team unit where Patient A was being cared for when he died after suffering an epileptic seizure whilst bathing unsupervised. Patient A was a young man with learning disabilities, autism and epilepsy.
The main areas of concern (as found proven by the Tribunal) were her failures in:
- carrying out risk assessments or reviewing nursing risk assessments
- explaining the benefits, risks and side effects when prescribing Risperidone
- respecting best interests’ decision-making
- assessing Patient A’s mental state and formulating a diagnosis, aetiology and risk assessment when reviewing Patient A on occasions where a trigger event had occurred
- keeping adequate records
- meeting Patient A’s clinical needs by producing adequate care and treatment plans, both generally and in respect of epilepsy
- obtaining a history of Patient A’s epilepsy.
At a hearing before the Medical Practitioners Tribunal Service, the Tribunal found that Dr Murphy’s fitness to practise was impaired by reason of multiple failings in her care for Patient A and imposed a sanction of a 12-month suspension with review. We reviewed the case to come to a view about whether this sanction was insufficient to protect the public and whether Dr Murphy should have been removed from the GMC’s register.
Our scrutiny process involves a review of the initial published decision by a Tribunal, at which point concerns about the decision may be highlighted; then one of the lawyers within the team, or externally, will undertake a detailed review of the hearing transcripts and evidence placed before the Tribunal. Following this review a decision will be made by the Chief Executive as to whether or not to hold a Case Meeting. For the Case Meeting, we commission external legal advice in addition to considering the internal detailed case review. Two senior members of staff and a Board member will consider the case in detail and decide whether to make a referral to Court. We may refer a case to the relevant court if we consider that a relevant decision (a finding, a sanction, or both) is not sufficient for the protection of the public. You can find more information about our process and approach to our work under Section 29 on our website.
During this Case Meeting we identified a number of concerns about the Tribunal decision which included the following:
- There was a clear misunderstanding by the Tribunal of mental capacity law.
- There was reference in the decision to matters identified as mitigating factors which included that the Dr Murphy was a ‘young consultant in the difficult field of adult learning difficulties’ which could be read as suggesting that people with learning difficulties could receive a lower standard of care or reduce culpability for poor care. If this is what was meant it was plainly wrong. We considered that this reference to the nature of the patient group was inappropriate.
- The Tribunal did not consider whether Dr Murphy’s behaviour was fundamentally incompatible with continued registration.
However, we noted the Tribunal had closely examined Dr Murphy’s insight and remediation and had heard directly from Dr Murphy. The full case meeting note has been published on our website.
Taking all these matters into account, we considered that there was enough material before the Tribunal for it to decide that Dr Murphy was developing insight and that erasure was not the only sanction required in the public interest. In these circumstances, notwithstanding our concerns, we were unable to say that the sanction imposed by the Tribunal was insufficient.
 Find out more about our powers to appeal final fitness to practise decisions on our website or watch this short animation.
Find out more about our powers to appeal final fitness to practise decisions on our website or watch this short animation.
Issues highlighted in our annual report 2017/18 on fitness to practise
We have just published our annual report for 2017/18. In the report, we take the opportunity to look back at what has been achieved over the last 10 years in professional regulation, as well as providing our overview of how the regulators are performing.
We note that it is performance against the Fitness to Practise Standards that the regulators find the most challenging. Many of the regulators are trying to find ways to improve the way they deal with fitness to practise complaints. Though, we consider that innovations in the fitness to practise process can be valuable, if implemented appropriately, we believe that it is also important that such processes should not be used in a way which results in serious matters not being adequately investigated.
Our scrutiny of final fitness to practise decisions also gives us a wide perspective, allowing us to identify common issues across the regulators. This year we noted our concerns relating to:
- the duty of candour
- regulators’ prosecution of cases
- some regulators seeking to amend charges at the last minute
- a lack of detail in panel determinations making it difficult to understand the reasoning behind the panel’s action
- panels do not seem to appreciate the importance of whistleblowing
- the fact that panels are considering that where no actual harm has occurred as a mitigating factor when it should be treated as neutral
- a failure to adopt the approach that sexual motivation is a matter of inference, based on all the evidence
- the NMC’s finding of no misconduct in cases where its registrants have assaulted patients with challenging behaviour
- the possibility of the duplication of costs and efforts from the GMC’s right of Appeal under section 40A of the Health and Social Care Act
- the loophole in the NMC’s legislative framework allowing it to remove individual registrants from its register before the High Court can address our referral
- cases where a registrant decides to retire/cease practice.
Find out more in our full report, or our highlights report for 2017/18.
Performance reviews
Reviewing the Standards of Good Regulation
We have just launched a second consultation as part of our review of the Standards of Good Regulation and are now seeking feedback on the detailed proposals.
The Standards of Good Regulation are the tools that we use to inform our assessment of how the regulators that we oversee are carrying out their duties to protect the public. The current Standards have not been changed since 2010 and we considered that it was time to review them.
We first consulted on this last year to seek views about the general scope of the Standards and the matters that we should be examining. We received 29 responses to that consultation and also held workshops with key parties, including the regulators. This feedback has helped us draft our new proposed Standards of Good Regulation.
We hope that the new Standards will remove duplication and will provide greater flexibility for the regulators to develop their processes. The proposed Standards also look at the way in which regulators monitor their own performance and ensure that the different parts of the organisation are working together to protect the public.
We are keen to hear from the regulators and other stakeholders about the proposed Standards, as well as the evidence we will require regulators to provide to demonstrate how they are meeting them.
The deadline for responses is 10 September 2018. You can read the consultation paper, the proposed new Standards and the evidence framework on our website as well as a blog from our Director of Scrutiny and Quality who explains more about why the time is right to review the Standards.
Latest performance reviews published
Our two latest reviews are for:
- The Nursing and Midwifery Council for 2016/17 – which met 23 out of 24 Standards of Good Regulation. We held this review back until we had completed our lessons learned review. The issue we underscored heavily in that review – about how the NMC treated and communicated with patients and their families is one we still feel has not been addressed. We would like to see an improvement in the NMC’s approach to how it values evidence from, and communicates with, patients and their families. We would also like to see a greater commitment in practice to transparency.
- The Health and Care Professions Council 2017/18 – the HCPC has engaged positively with the findings from our 2016/17 review in which we highlighted numerous concerns relating to their performance against the Standards for Fitness to Practise – failing to meet six out of 10 of them. In our 2017/18 review, we did not find enough evidence of sustained improvement to be able to say that the HCPC had met them for, but we acknowledge the progress already made and its implementation of a long-term action plan to address the issues.
Both reports are available to read on our website along with two-page snapshot summaries (for the HCPC and the NMC).
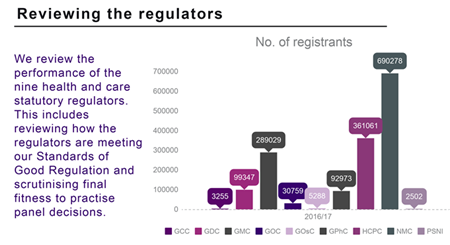
Reviewing the regulators – key stats for 2017/18
We have just published our annual report. You can read through our highlights and key statistics for our performance review and scrutiny and quality teams in this infographic.
